When babies cannot feed at the breast comfortably and effectively, and breastfeeding support is hard to find or not able to help, mothers may choose to use a breast pump to express all the milk their baby needs, and then feed via a bottle or feeding tube. This is known as exclusive pumping. While this is often a temporary solution to protect milk supply until the baby is able to nurse directly at the breast, some mothers may find themselves exclusively pumping long term. Some mothers may also actively choose to exclusively pump and some mothers may be unable to feed their baby directly at the breast because their baby is poorly or has medical difficulties.
The decision to exclusively express breastmilk usually stems from an awareness of the irreplaceable qualities of breastmilk. Mothers also find that providing their babies with breastmilk can help with the grief from not being able to nurse directly at the breast. If their baby has medical difficulties, many mothers feel strongly that providing human milk will give their child the best possible start, particularly if their baby is in hospital. Yet, exclusive pumping is a significant undertaking which requires dedication, information and support.
You might find the decision to exclusively express feels difficult, and that you don’t feel you fit with breastfeeding mothers or with those using formula. Please be sure that you will receive a warm welcome and support at LLL meetings and from your local Leader, and that we understand the lengths you’re going to, to make sure your baby has your milk.
This page concentrates on the practicalities of how and when to express your milk and feed it to your baby, to establish exclusive expressing as your feeding method. Sometimes it can help to focus on all these practicalities and, once you have a workable plan, to give yourself time too to process how you’re feeling about it, as you settle into life with your new baby. If you have a partner or supporter at home with you, all the things that are useful in supporting a breastfeeding mother will apply to you too!
Getting Started
Equipment
Setting your schedule
How long is an expressing session?
The importance of Oxytocin
How to pump
How much milk to pump
Feeding your breastmilk
Storing your breastmilk
Stopping exclusively pumping
Getting Started
If you have recently given birth and your mature milk has not yet come in, hand expressing is the most effective way of collecting colostrum to feed to your baby. It is important to start expressing colostrum within six hours (ideally after one hour, if possible) of giving birth, though if this doesn’t happen for you, it is still possible to get started.
A newborn would expect to feed 8-12 times in 24 hours, and the feeds might not be evenly spread over that time, though they do need to include some feeds in the night; it is important to try to express breastmilk just as frequently in order to lay the groundwork for a robust milk supply later on. If you can have skin to skin contact with your baby while you’re expressing, it can really help, and a photo or something that smells of your baby can be a substitute. You can collect your colostrum in a syringe, a small clean cup or a spoon. See our article on Hand Expression of Breastmilk for more information on hand expressing, and you might also find this video on hands-on pumping helpful. This technique can be tricky to get the hang of, so please do ask your midwife or other breastfeeding supporter to help. It’s very common to need an extra pair of hands to collect the drops of colostrum.
Equipment
As your milk starts to transition, you will probably notice it start to change colour and spray out as you are expressing; this is a good time to introduce a breast pump. Although some women respond better to hand expressing, using a hospital grade double electric pump is the most effective way of removing breastmilk when a baby isn’t latching or is not nursing adequately. If you are planning on exclusively expressing for your baby long term, then it will be worth investing in a hospital grade double pump. If you would like to try one before deciding whether or not to buy it, your hospital or midwife may be able to provide you with one on a short-term loan. Alternatively, you can hire a pump, although it may turn out to be rather expensive if you are exclusively expressing long term.
A breast pump usually comes with a collection set and the part that sits over your nipple/areola, which is called a flange. As women’s nipples and skin elasticity differ, flanges are available in different sizes. It’s important to ensure you have the right size for your nipples, as flanges that are too large or too small may cause pain or nipple damage and reduce the amount of milk you are able to express. Finding the right flange size may be a bit of a trial and error process; you may want to start by trying the standard size that comes with the pump (which varies for different pump brands) and see how you respond. If the standard flange sucks in too much areola, or if your nipple is at the back of the pump, you may need to go down a size. If, instead, you are left with a white ring around your nipple, you may need to go up a size.
Many mums find being able to express handsfree invaluable in terms of allowing them to fit regular pumping sessions into their day. There are a small variety of pumps that provide milk collection cups that sit inside your bra, freeing you up to cuddle your baby without fear of spilling your milk. However, they tend to have a limited range of flange sizes. Alternatively, you can buy special bras designed to hold your pump flanges against your breasts, or you can even DIY your own by cutting holes in a stretchy bra that line up with your nipples.
There are several other things to consider when choosing which hospital grade double pump to purchase or hire:
– How often will you use it? If you are planning to exclusively pump long term, you may need to consider motor life, to make sure the pump you purchase will live up to its use.
– How portable is it? If it uses a battery, then it can be carried around the house or out and about with you. Some pumps have built-in rechargeable batteries, while others offer the option to purchase a power pack or a car charger. Some pumps use removable batteries which are easy to replace if you unexpectedly run out of charge while away from a plug socket. However, using removable batteries may end up being rather expensive long term. You might find you end up using two different pumps – an efficient hospital grade one when you’re at home and a hand pump or battery pump when you’re out and about.
– Can you purchase spare collection sets? Having a spare collection set or two can come in handy, as most mothers find that it is easier to stick to their pumping schedule if their pump is set up and ready to go at a moment’s notice, especially at nighttime.
Setting your schedule
For the first three-four months, you will need to express regularly to build a robust milk supply, ideally 8-12 times in 24 hours. Although you do not always need to pump at regular intervals, it is best not to go more than two to three hours between pumping sessions, with one longer stretch of four-five hours at night if you can take this break without damaging your milk supply. You will need to have at least one pumping session overnight, ideally between 2am and 5am when prolactin levels are highest. If you are able to pump when your baby wakes up for a feed, you may find it easier to do so than setting an alarm. If you need to set an alarm, but are having difficulty waking up, it may be worth experimenting with setting it for different times to try and coincide with the periods in your sleep cycle where you are in a lighter sleep. Many mothers find that they are able to express the most milk first thing in the morning, and less as the day goes on. You will notice your own patterns. It’s also common for one breast to produce more milk or have a faster flow than the other side.
Working out ways to fit pumping sessions into your routine is key to long-term success. Some mothers will express while cooking, or holding a sleeping baby, or while travelling; sometimes before they feed their baby, sometimes afterwards. Experiment to find out what works best for your family and your daily rhythms.
In the early days, you may find that you are producing more milk than your baby needs; this is common and it will settle down in a few weeks. It can be useful to freeze any excess milk in small portions for later on, should your baby suddenly require more milk, such as during a growth spurt or period of illness.
Once your supply has established, usually between three and four months, you may decide to slowly reduce your number of daily pumping sessions. If you are planning to exclusively express long term, however, you may decide not to make any changes to your pumping schedule. If you start to reduce your expressing sessions, you may like to keep a record of your daily pumping outputs so that you can monitor what effect it has on your overall milk supply. You could start by increasing the intervals between your overnight pumping sessions, although it will still be important to express once at night. After doing this for about three-four weeks, you may consider dropping one daytime session. This may require you to adjust the time of all your other pumping sessions, in order to avoid leaving a big gap in between them, which could make you vulnerable to experiencing blocked ducts or mastitis.
Once your baby starts eating solids reliably, around eight-nine months, you may start to notice a change in their milk requirements and can adjust your pumping schedule and milk supply accordingly. However, many mothers find that introducing solids does not affect milk intake for a lot longer (in some cases, 18 months). When your baby is sat in a highchair, it can be a good time to express your milk without them pulling on the pump tubes.
How long is an expressing session?
The length of each expressing session will vary for each mother, based on her breast storage capacity and the type of pump she uses. If you are able to express milk from both breasts at once, then you will find it much faster.
While some experts recommend pumping for about 15-20 minutes, others believe that specifying the duration of a pumping session may not be helpful, as some mothers may take up to 45 minutes. In her book Exclusively Pumping Breastmilk,i Stephanie Casemore suggests spending two hours over the course of 24 hours expressing. However, this total pumping time may need to be adjusted for mothers who need long individual expressing sessions. Also, other experts believe the total number of separate sessions to be more important than total pumping duration, with shorter, more frequent expressing sessions usually being more effective than fewer, longer sessions.
As a general rule of thumb, you can express until your milk stops spraying, and then for an additional five minutes to stimulate another let-down. If you need to increase your supply, you can pump for 10 more minutes and use hand expression right after to remove as much milk as possible. Breast compressions and massage during sessions (hands-on pumping) also help to stimulate let-downs and maximise milk output. Some mothers find that it helps to experiment with “power pumping”, where they pump frequently for short periods, to mimic cluster feeding. This might be something to use on occasion rather than as part of a daily routine as it can be quite time-intensive.
If, on the other hand, you need to decrease your supply, then slowly reduce the length of time you are expressing for. In both cases, many of the techniques discussed in our articles “My baby needs more milk” and “Too Much Milk and Oversupply” can be adapted for use with a breast pump.
If you are worried that you do not have enough time to do a full session, then it is better to pump less time and have a longer session later, than to miss one entirely.
Over time, as you reduce the number of pumping sessions, you may find that you will need to express for longer to obtain the same amount of milk. Many women find that if they cycle through their pump settings again, they can trigger a second or even a third let-down over a period of 30-45 minutes.
The importance of Oxytocin
Oxytocin is the hormone that triggers your letdown (milk ejection reflex). It is especially important to be mindful of this when expressing, as even mildly stressful situations of feeling rushed can make it difficult to trigger a letdown when using a breast pump. Many mothers find looking at their baby – or at pictures of their baby if they are separated – while expressing helpful. Gently massaging your breasts before and during your pumping session, as well as applying warm compresses or taking a warm shower before expressing can also trigger a let-down. Other ways to boost your oxytocin might include listening to music, watching a comedy on TV, reading a book, or browsing social media on your phone.
If you are able to cuddle your baby while expressing, you may see an increase in your normal milk output! It is even possible to express while carrying your baby in a sling or baby carrier. As your baby gets older and more mobile, you may find it easier to remove yourself to a different room where you can relax without worrying about them pulling on your tubes, or getting into things they shouldn’t.
It can feel disheartening if you are watching your collection bottles and feel that they are not filling up quickly enough. Covering the bottles with socks, or distracting yourself so that you are not watching, can be helpful. If you are struggling to get a let-down, it is ok to put your pump away and come back to it 10-20 minutes later and try again. If it is a persistent problem at certain times of day, try to remember that the stimulation you are giving your breast still has a valuable purpose.
How to pump
In order to keep pumping comfortable and avoid nipple damage, you may want to consider using lubrication, such as lanolin or olive oil, inside the pump flange to reduce friction. The flange needs to make a comfortable seal around the breast.
Pumps have different suction and cycles settings. You may want to start with a low suction and high number of cycles to stimulate your let-down. Once your milk starts flowing, you can decrease the number of cycles and increase suction. In order to avoid getting sore, it is a good idea not to use the same suction setting for long periods of time. Switching between low and high suction also helps to trigger more let-downs.
Once you are done pumping, you can massage both breasts and hand express to make sure your breasts are completely drained.
How much milk to pump
As breastmilk is highly digestible, breastfed babies tend to feed little and often. When babies nurse directly at the breast, milk intake varies from feeding to feeding, so the amount of breastmilk taken per bottle may also vary throughout the day. On average, babies need 750-1035ml of breastmilk per day between one and six months of age. You may want to pump slightly more than this to make sure you have enough milk when your baby goes through a grow spurt.
Feeding your breastmilk
Babies drink from a bottle and nurse from the breast in a completely different way. When drinking from a bottle, babies cannot control the flow of milk, which can be uncomfortable for them and can lead to overfeeding. In order to minimise this problem, you may want to feed your baby your expressed milk in a way that is as close as possible to nursing. This is often referred to as paced bottle feeding.
Rather than feeding your baby bottles of expressed milk according to a strict schedule, you may want to feed on demand, as you would if they were nursing at the breast, being aware of early hunger cues. Holding your baby upright and keeping the bottle in a horizontal position allows the baby to suck actively, as he would at the breast, and to control the flow of milk, taking a break whenever he needs to. Offering the bottle teat gently, letting the baby draw it into their mouth, and feeding to satiation also allow the baby to be more in control of his feed. You can find more information on how to feed your baby your expressed milk in our article ‘Bottles and other tools‘.
It’s important to remember that breastmilk should not be warmed up in a microwave or in a pan on the hob, in order to avoid damaging its nutrients. Shaking breastmilk is also not necessary.
Storing your breastmilk
Breastmilk’s antibacterial properties help it stay fresh, so it can be safely stored at room temperature for four-six hours and in the fridge for up to a week. If away from home, you could use a cool bag with ice packs. Our page Storing Your Milk has comprehensive details on safe periods for storing expressed milk for healthy babies. If your baby is unwell or premature, then follow hospital guidelines. Your baby will benefit more from fresh than frozen breastmilk because its living properties will help him fight off possible infections, however all human milk is beneficial for you baby.
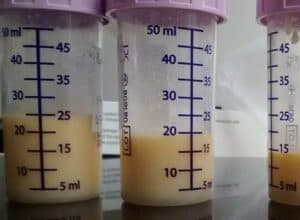
You may well see that your expressed milk is not always the same colour, and that it separates into layers when it has been stored for a while. Neither of these is a cause for concern, and a gentle swirl of the container before you feed your milk to your baby should make the layers mix again.
If you find that you are producing more milk than your baby needs, you might like to consider donating your milk by registering as a donor for your local breastmilk bank.
Stopping exclusively pumping
When you feel ready to stop expressing milk for your baby, it’s important not to rush into dropping pumping sessions, in order to avoid the risk of experiencing blocked ducts or mastitis. Your breasts need time to adjust, so it’s best to adopt a gradual approach. You could try to reduce the length of your pumping sessions by a few minutes over a few weeks, or you could try slowly increasing the intervals between sessions.
Exclusive pumping, while also doing the day to day work of looking after your baby, can be exhausting, and sometimes mothers and parents wrestle with feeling guilty about having stopped “too soon”. By taking on the work of exclusive pumping, though, you gave your baby a wonderful gift.
Written by Nicola Sheldon (LLL Berkshire and Oxfordshire) and Eva Williams (LLL Oxfordshire), May 2020.
Thanks to Harriet Valentino for her input and to Lois Rowlands, Rae Vacher Lowe and Laura Loasby for the photos.
Further reading
https://laleche.org.uk/hand-expression-of-breastmilk/
https://laleche.org.uk/my-baby-needs-more-milk/
https://laleche.org.uk/too-much-milk-and-oversupply/
https://laleche.org.uk/bottles-and-other-tools/
https://laleche.org.uk/expressing-your-milk/#Pumps
https://laleche.org.uk/storing-your-milk/
A mother’s story from our members magazine breastfeeding matters
https://kellymom.com/category/bf/pumpingmoms/pumping/
Exclusively Pumping Breastmilk, Second edition. Casemore, S. Gray Lion Publishing, 2014
i Exclusively Pumping Breastmilk. Second edition. Casemore, S. Gray Lion Publishing, 2014